| Symptoms of SBS |
| Subdural Hematomas |
Retinal hemorrhage means bleeding onto the surface of the retina (visual receptor of the eye) caused by rupture of the tiny blood vessels that lie on the surface of the retina. Retinal hemorrhage means extremely violent force to the head; it is essentially diagnostic of the shaken baby syndrome of child abuse. Retinal hemorrhages are not seen after falls to the floor from the changing table, or falling from waist level!!( information from sleeptight.com)
Robert W. Enzenauer, MD, MPH
FAAO, FAP, FACS
Pediatric Ophthalmology and Adult Strabismus
Chattanooga, TN
| Subdural Hematomas |
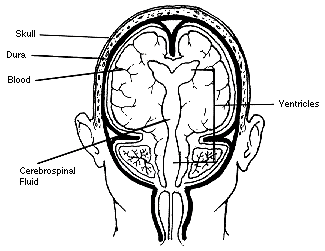
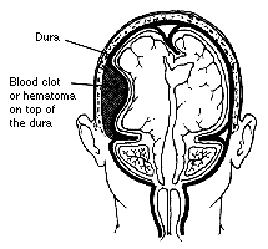
Pictures from Children's Virtual Hospital
Subdural means "below the dura" (the dura mater is the outer membrane covering the brain). Subdural hematoma develops when blood veins that are located between the membranes covering the brain (the meninges) leak blood after an injury to the head .
Blood collects into a mass (hematoma) that presses on the tissues of the brain. Pressure damages the brain tissue and causes loss of brain function that may progressively worsen as the hematoma enlarges and intracranial pressure (pressure within the head) increases. The injury and the resulting collection of blood cause inflammation of the brain tissues, which leads to swelling (cerebral edema). Cerebral edema further increases the intracranial pressure.
Subdural hematoma often develops as a complication after a head injury. Symptoms of subdural hematoma may develop even after symptoms of the head injury (such as decreased consciousness ) have improved. Acute subdural hematoma progresses rapidly, with symptoms usually appearing within 24 hours of the injury. Rapid deterioration occurs thereafter. Acute/sub acute subdural hematoma is less common, but more often fatal, than chronic subdural hematoma .